- Automatic mode switch for atrial arrhythmias
- Other specific algorithms of atrial arrhthmias management
1- Automatic mode switch for atrial arrhythmias
Mode switch is an ON / OFF programmable function designed to prevent the tracking of paroxysmal atrial tachycardias when the pacemaker operates in DDD, VDD or MVP modes.
Mode switch to non-atrial tracking mode (DDD to DDIR)
The criteria prompting a switch from an atrial synchronous to DDIR mode vary among the range of implanted pacemakers. In the Adapta series, the pacemakers switch to DDIR mode when:
- out of 7 consecutive atrial intervals (AS-AR or AR-AS), 4 are shorter than the programmed detect rate interval.
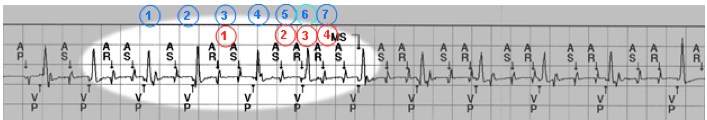
In the Advisa / Ensura series the pacemaker switches to DDIR mode when 1 or both the following conditions is (are) met:
- the median of 12 consecutive atrial intervals is shorter than the programmed AT/AF interval.
- The AT/AF counter is ≥3. The AT/AF counter of is incremented by 1 point, each time ≥2 atrial events are sensed between 2 ventricular sensed or paced events.
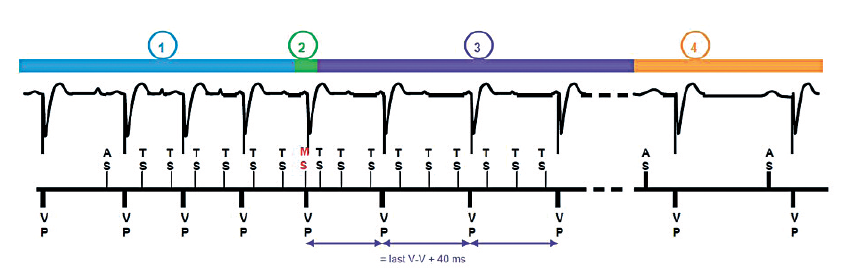
- Onset of atrial arrhythmia in a patient in complete AV block, programmed in DDD mode. Each AS event is followed by a ventricular paced event: acceleration of the pacing rate.
- The AT/AF counter = 3 (3 VP-VP cycles with at least 2 sensed atrial events): mode switch to DDIR (MS).
- Gradual slowing of the tracking rate to the rate responsive rate (+ 40 ms with each interval)
- End of arrhythmia. Return to the programmed mode (except for the MVP mode with which there is invariably a return to DDD preceding the return to AAI)
Mode switch to atrial tracking (DDIR to DDD or VDD)
The criteria which lead to the switch from DDIR to the atrial synchronous mode also vary depending on the series of pacemakers implanted.
With the Adapta models, the pacemaker switches to the atrial tracking mode:
- if the last 7 A-A intervals are longer than the maximum synchronous rate interval, or if 5 atrial pacing events occur.
With the Advisa / Ensura series, the pacemaker switches to the atrial tracking mode if 1 of the following criteria is met:
- identification of normal sinus rhythm (or normal paced rhythm) for 5 consecutive ventricular intervals
- the median atrial cycle is longer than the AT/AF sensing cycle
- the AT/AF counter is <27 for 3 min.
In both series, the ventricular pacing rate switches from sensor-indicated to atrial tracking.
Blanked flutter search
The mode switch algorithm has a programmable blanked flutter search setting based on the detection of short atrial cycles occurring on a 2:1 basis in the PVAB. Atrial flutter is a perfectly regular arrhythmia.
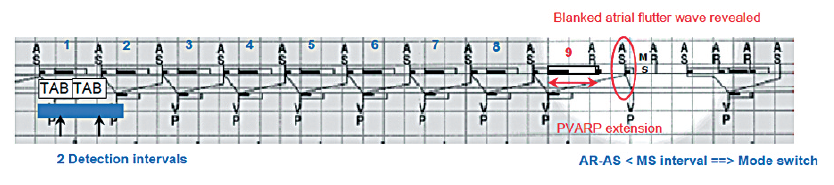
Depending on its rate and on the setting of the AV delay, 1 out of 2 atrial events may fall in the PVAB. Consequently, 1 out of 2 flutter waves is labeled AS and is followed by pacing, while the other atrial event falls in the PVAB and is neither sensed nor counted by the device. This may continue and cause a prolonged, rapid ventricular paced rhythm without diagnosis of flutter. The algorithm of blanked flutter search is activated when 8 consecutive AS-AS intervals are:
- shorter than twice the sum of the AV delay + the PVAB;
- shorter than twice the programmed interval of atrial arrhythmias detection.
If these 2 conditions are met, the device suspects the presence of blanked flutter and extends the PVARP of the next cycle to unmask the next atrial event (AR) in the refractory period, suppress ventricular pacing and uncover the next flutter wave (AS).
Memorization of atrial arrhythmia episodes
Pathologic atrial events are memorized when they cause fallback. Fallback and memorization are, therefore, coupled.
2-Other specific algorithms of atrial arrhythmias management
Non-competitive atrial pacing (NCAP)
Aim: to prevent the triggering of an atrial tachyarrhythmia by an atrial pacing stimulus that falls within the atrium’s vulnerable period.
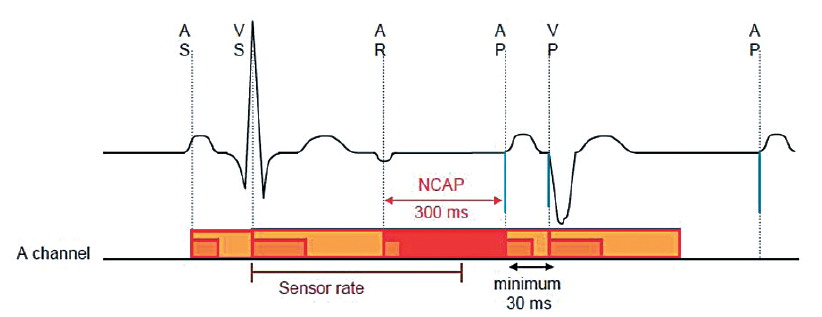
Operation: when NCAP is programmed ON, a sensed atrial refractory event falling in the PVARP starts a programmable NCAP during which no atrial pacing may occur. If a sensor-driven or a lower rate pacing stimulus is scheduled to occur during the NCAP, the VA interval is extended until the NCAP expires.
If no pacing stimulus is scheduled to occur during the NCAP, the timing is unaffected and pacing occurs at the end of the VA interval, unless inhibited. An atrial refractory sensed event occurring during the NCAP starts a new NCAP.
When an atrial pacing stimulus is delayed by the NCAP operation, the pacemaker attempts to maintain a stable ventricular rate by shortening the paced AV delay that follows, down to a minimum of 30 ms. The paced AV delay, however, will not be shortened beyond 30 ms. The NCAP interval is 400 ms for 1 paced cycle each time a PVC response or an anti-PMT intervention occurs.
This function is available when the pacemaker operates in DDD, DDI, or MVP (AAI<=>DDD) modes.
Atrial preference pacing
Aim: Atrial preference pacing (APP) is designed to lower the incidence of atrial tachyarrhythmias by forcing atrial pacing at a rate slightly higher than the spontaneous rhythm.
Operation: the device responds to variations in the atrial rate by accelerating the pacing rate until it reaches a stable paced rhythm that is slightly faster than the spontaneous rate. After each sensed, non-refractory atrial event, the device shortens the atrial pacing interval by a programmed decremental value. If the next atrial event is another non-refractory sensed event, the pacing interval is further decremented. This overdriving function continues until the pacing rate surpasses the spontaneous rate, resulting in a paced atrial rhythm. However, the programmed upper rate provides a limit to the APP rate. After a programmable period of atrial pacing at 100%, the pacemaker gradually decreases the pacing rate, like a smoothing function, in search of the next spontaneous sinus cycle, which restarts the APP.
A long decremental interval causes a more aggressive response to a sinus rate increase, which means that APP occurs more often, more rapidly and lasts longer than with a shorter decremental interval. Conversely, a shorter interval attenuates the response to isolated atrial extrasystoles and sinus variability near the lower rate. APP reacts more slowly to a sustained increase in rate. APP is available when the pacemaker operates in DDD, AAI or MVP mode.
The atrial pacing pulses delivered by APP are labeled PP (proactive pacing) on the event markers.
Atrial rhythm stabilization (limited to the Advisa series)
Aim: atrial rhythm stabilization (ARS) is a programmable function designed to prevent long sinus pauses, which usually follow atrial extrasystoles. Short-long-short cycle sequences can be arrhythmogenic and facilitate the onset of atrial tachyarrhythmias.
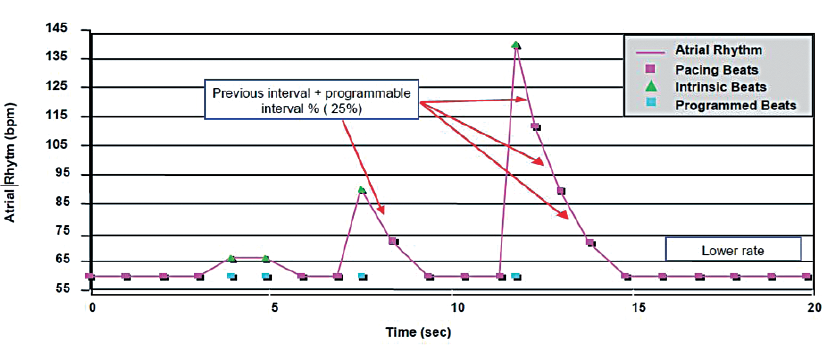
Operation: when activated by the sensing of an atrial extrasystole, the device delivers a pacing pulse at the premature interval, increased by a percentage of that interval (defined by a programmed Interval Percentage Increment parameter). The atrial pacing rate is then gradually decreased until the return of the spontaneous rate, the programmed pacing rate or the sensor rate. The Maximum Rate parameter sets an upper rate limit for ARS.
ARS is available when the device operates in DDD, AAI or MVP (AAI<=>DDD) mode.
The atrial pacing pulses delivered for ARS are labeled PP (proactive pacing) on the event markers.
Post mode switch overdrive pacing (Adapta and Advisa series)
Aim: post mode switch overdrive pacing (PMOP) can be added to the mode switch function to pace the atria rapidly after the cessation of an episode of atrial tachyarrhythmia. The emergence of a slow heart rate after the end of an arrhythmia is associated with an increased risk of very early recurrence.
Operation: after the return of sinus rhythm and switch to DDD/VDD mode, the device increases the pacing rate beat-by-beat (decreasing the pacing interval by 15 ms per pulse for Adapta and 70 ms for Advisa) until it reaches the programmed Overdrive Rate. It then smooths the return to the programmed atrial tracking mode by gradually slowing the rate until reaching the programmed pacing rate, the lower programmed rate or the sensor rate.
PMOP is available when the device operates in DDD or MVP (AAI<=>DDD) mode.
Reponse to conducted AF (Adapta and Advisa series)
Aim: the response to conducted AF is an algorithm designed to promote a regular ventricular rate during episodes of AF to prevent long diastoles.
Operation: during an episode of AF, the pacemaker modifies the beat-by-beat pacing rate in order to pace near the mean intrinsic ventricular rate. This eliminates long pauses and diminishes the irregularity of the ventricular rate. The response to conducted AF function adjusts the pacing rate, such that it is faster in presence of sensed ventricular events and slower in presence of ventricular pacing pulses. The increase in pacing rate caused by the response to conducted AF is limited by the programmed maximum rate. Depending on the programmed response level value (a higher response level value results in a higher percentage of ventricular pacing and faster alignment with the patient’s own ventricular response rate), the device accelerates the pacing rate in response to a sensed event and slows the pacing rate in response to a pacing pulse.
The response to conducted AF functions only in non-tracking modes (VDIR or DDIR). To program the response to conducted AF ON, the mode switch.



