Dual chamber discrimination: V=A
Tracing
Manufacturer Abbott
Device ICD
Field Discrimination
N° 49
Patient
This 58-year-old lady received a St Jude medical Promote Accel CRT-D in the context of advanced idiopathic dilated cardiomyopathy with left bundle branch block and a history of AF ablation. She was seen in consultation, complaining of palpitations.
Main programmed parameters
- VF zone at 214 bpm, VT-2 zone at 164 bpm and VT-1 zone at 142 bpm
- 12 cycles in the VF zone, 12 cycles in the VT-2 zone and 12 cycles in the VT-1 zone were needed for the diagnosis
- Effective discrimination in the VT-1 and VT-2 zones
- V<A: if all criteria are fulfilled; morphology (60%, 5 out of 8), stability (50 ms, with 60-ms AV association delta, 12 intervals)
- V=A: if all criteria are fulfilled; morphology (60%, 5 out of 8), sudden onset (20%)
- Post-ventricular atrial blanking: 150 ms

Graph and trace
Narrative
Episode diagnosed as SVT in the V=A arm; in this patient, 2 out of 2 criteria are needed for the diagnosis of VT; both criteria (morphology and sudden onset) indicate SVT, the device diagnoses SVT and no therapy is delivered.
Tracing
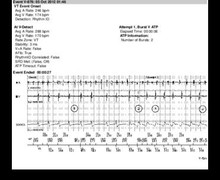
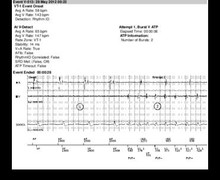
- tachycardia with 2 atrial for 1 ventricular event, though every other atrial event was not sensed because it fell in the post ventricular atrial blanking (thick line visible under the marker chain). The ventricular morphology is similar to that of the reference ventricular signal; the alternation of VS, unclassified cycles and T1 cycles without diagnosis of return to sinus rhythm is noteworthy; the tracing is consistent with probable atrial tachycardia (or flutter) with 2:1 ventricular response;
- after 12 cycles classified T1 (not all visible on this tracing) SVT is diagnosed in the V=A arm (=SVT); the alternation of VS, unclassified cycles and T1 cycles explains the absence of sudden onset; this is relatively common when the rate of the tachycardia, whether ventricular or atrial hovers around with slowest tachycardia zone. The morphology criterion is in favor of SVT, such that no therapy is delivered;
- after 6 T1 classified cycles, redetection and repetitive diagnosis of SVT;
- slight slowing of the ventricular rate and diagnosis of return to sinus rhythm (5 VS);
Other articles that may be of interest to you





Reliable sensing in both chambers is indispensable for the proper function of the dual chamber discrimination algorithms. Dislodgement of the atrial lead, cross-talk due to far-field sensing of the R wave in the atrium, undersensing of the atrial signals due to low-voltage signals during AF, and occurrence of the atrial activity in the post ventricular atrial blanking period may all be the source of inaccurate dual chamber discrimination.
This patient presented with atrial flutter and 2:1 ventricular conduction. The diagnosis of SVT made by the device was, therefore accurate. However, the classification in the V=A arm was erroneous, as every other atrial event occurred in the post ventricular atrial blanking period. This episode should have been classified in the V<A arm. An excessively long post ventricular atrial blanking period, as was programmed in this patient, limits the proper counting of the atrial signals by the device. It would likely have been appropriate to shorten this parameter to a more usual value, between 50 and 80 ms.