Limitations of the dual-chamber VDD mode
Tracing
Manufacturer Biotronik
Device PM
Field Pacing Modes
N° 8
Patient
Young patient, 21 years old, implanted with a VDD pacemaker at the age of 11 for a congenital atrioventricular block; replacement of the pulse generator 3 years ago with implantation of an Evia DR-T pacemaker; programming in VDD mode 60 bpm; transmission of a periodic EGM by remote monitoring.
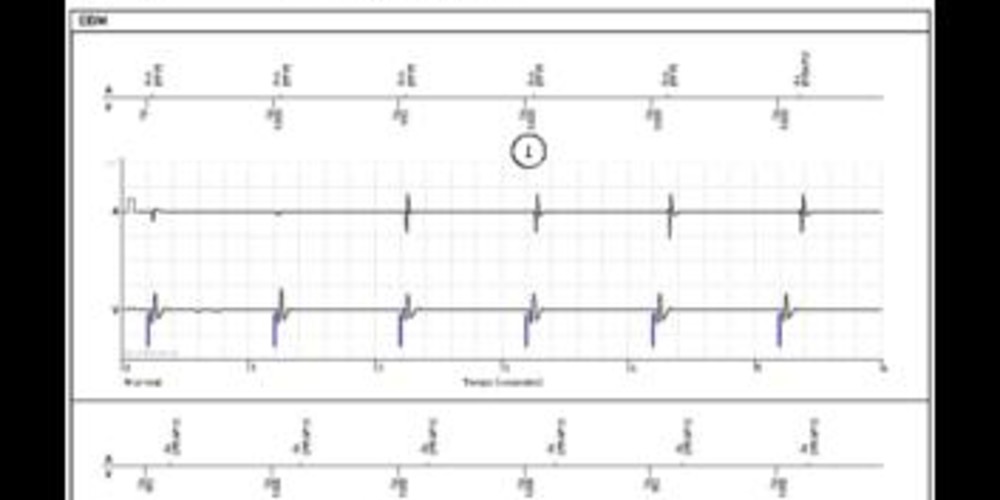
Graph and trace
Normal: programming in VDD mode 60 bpm;
- ventricular pacing at 60 bpm and sensing of sinus rhythm in the post-ventricular atrial "blanking" period (far-field protection, PFF);
- sinus activity sensed in the PVARP;
Encouraged sensing: automatic slowing of the base rate;
- sensing of sinus activity and ventricular synchrony (AS-VP);
Encouraged pacing: VDD mode at 60 bpm;
- new loss of atrioventricular synchrony, the sinus rhythm being slower than the minimum rate.
Other articles that may be of interest to you




The VDD mode can be programmed on a traditional dual-chamber pacemaker but can also be obtained from a single-lead VDD dual-chamber device with two pairs of electrodes, one floating atrial pair providing atrial sensing, and one ventricular pair for ventricular pacing and sensing. On the other hand, atrial pacing is not possible. This mode is therefore acceptable in the absence of sinus dysfunction, and a low base rate should be programmed, possibly with rate hysteresis, in order to avoid VVI behavior. Indeed, on this tracing, the programming at 60 beats/minute is associated with a loss of atrioventricular synchrony.
The advantages of single-lead VDD systems are that
The disadvantages of single-lead VDD systems are that
The preferred indication of the VDD mode is therefore complete atrioventricular block with normal sinus function.
In this patient, the recording of this periodic EGM led to a reduction of the minimum rate in order to promote atrial sensing.