Medtronic - MVP
Content
MVP (Managed Ventricular Pacing)
The MVP (Managed Ventricular Pacing) mode is an atrial-based pacing mode designed to promote intrinsic conduction and to reduce the percentage of unnecessary right ventricular pacing.
Operating details
MVP provides the following functions:
- AAI mode pacing when AV conduction is intact
- backup ventricular support for transient loss of AV conduction
- ability to automatically switch to DDD pacing during sustained AV block
- periodic conduction checks at progressively increasing intervals while operating in DDD mode, with the ability to switch back to AAI mode when AV conduction resumes
Intact AV conduction
The MVP mode, AAI<=>DDD, provides AAI mode pacing while monitoring AV conduction (ADI mode). If AV conduction is intact, the device remains in AAI mode. While operating in AAI mode, the parameters associated with single chamber atrial pacing are applicable.
Transient loss of conduction
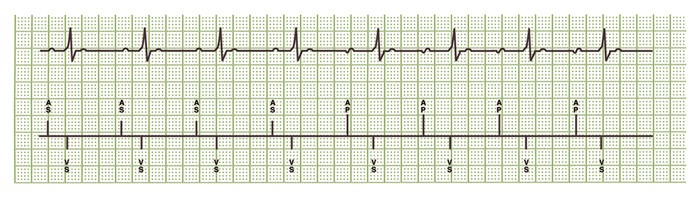
For transient loss of AV conduction, the device remains in AAI mode and provides a backup ventricular pacing pulse in response to an A-A interval that is missing a ventricular sense.
In this example, ventricular backup pacing occurs 80 ms after the scheduled AP on the next cycle following A-A intervals without a valid ventricular sense. The device does not switch to DDD after a single A-A interval without a valid ventricular sense.
Sustained loss of AV conduction
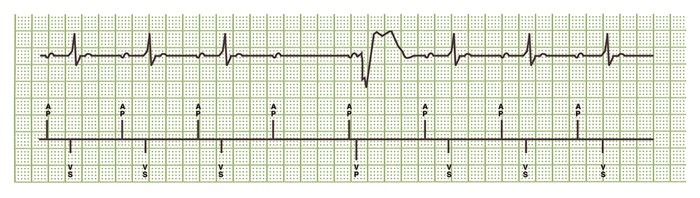
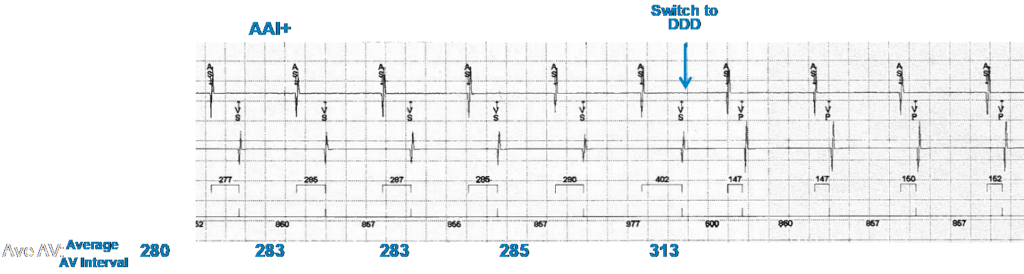
When no ventricular sensed event occurs in 2 of 4 preceding A-A intervals, the pacemaker automatically switches from AAI to DDD mode.
In this example, ventricular backup pacing occurs 80 ms after the scheduled AP following each A-A interval without a valid ventricular sense. The pacemaker switches to DDD mode since two of the most 4 recent non-refractory A-A intervals are missing a ventricular event.
AV conduction resumes
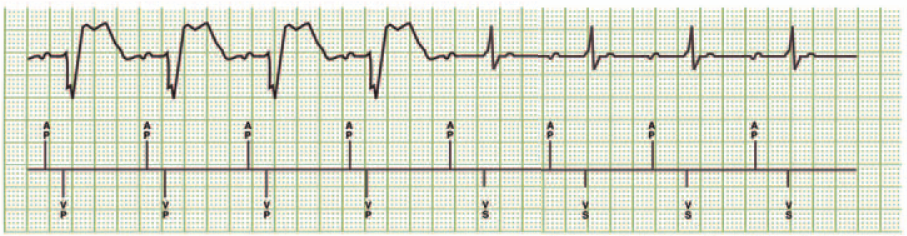
After switching to DDD mode, the device periodically checks AV conduction for an opportunity to return to AAI mode. The first AV conduction check occurs 1 minute after switching to DDD mode. During the conduction check, the device switches to AAI pacing mode for one cycle.
If the next A-A interval includes a sensed ventricular beat, the conduction check succeeds. The device remains in AAI pacing mode.
This tracing shows one example of successful conduction check after one minute of DDD pacing.
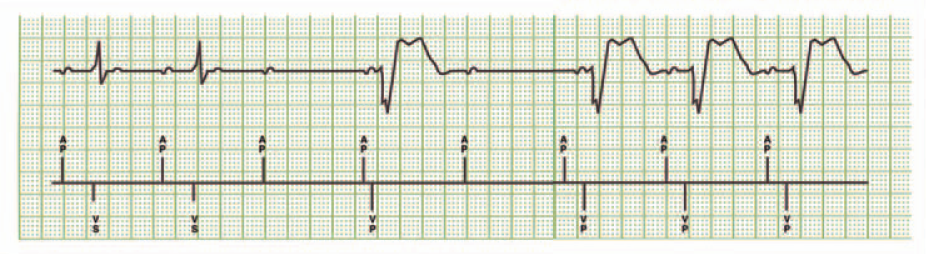
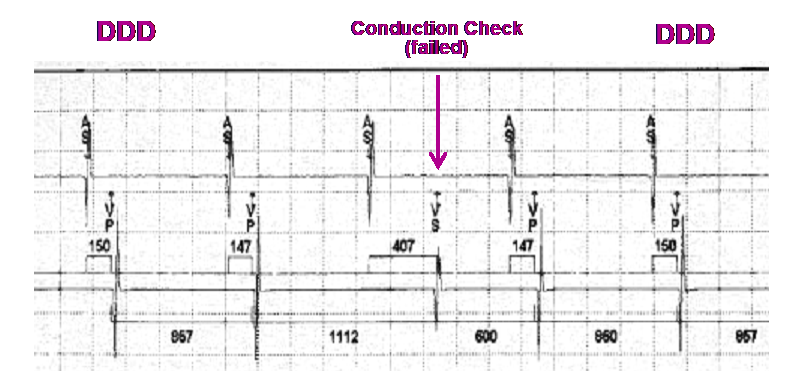
If the next A-A interval does not include a sensed ventricular beat, the conduction check fails, and the device switches back to the DDD mode. The time between conduction checks then doubles (2, 4, 8 … minutes, up to a maximum of 16 hours) with each failed conduction check.
Specificities of the algorithm
Atrial Refractory Period: when MVP is operating in AAI mode, the Atrial Refractory Period is not programmable. Instead, it is automatically adjusted according to the current heart rate: 600 ms for rates below 75 bpm and 75% of the ventricular interval for rates at or above 75 bpm. An atrial activity detected in this dynamic Atrial Refractory Period does not reset the A-A escape interval to avoid inappropriate switches to DDD in the presence of non-conducted premature atrial contractions.
PVCs and ventricular tachyarrhythmias: because cross-chamber blanking may affect sensing of ventricular arrhythmias, when MVP is operating in AAI mode, the device inhibits atrial pacing in response to PVCs, PVC runs, and ventricular tachyarrhythmia episodes. This behavior is intended to prevent unnecessary atrial pacing when the ventricular rate is faster than the pacing rate. It also allows tachyarrhythmia detection features to operate without disruption from blanking periods caused by atrial pacing.
Ventricular pause and lower rate limit: upon abrupt loss of AV conduction, prior to switching to DDD mode, the MVP mode allows the occurrence of occasional pauses of up to twice the programmed lower rate interval. It is therefore recommended to program the Lower Rate to 50 bpm or higher to decrease the duration of the pause in case of loss of atrioventricular conduction.
Complete heart block: for patients with complete AV block, the device operates in DDD mode persistently. Every 16 hours, the device checks for AV conduction, which results in a single dropped ventricular beat. If this pause is symptomatic, programming of the DDD mode may be more appropriate.
Long PR intervals: for patients with long PR intervals, the device remains in the AAI mode. Permanent DDDR or DDD modes may be more appropriate for patients with symptomatic first-degree AV block particularly if there is no reduction of the PR interval during exercise.
Operation immediately after implant: the device is shipped in MVP mode, initially operating in DDD mode. Approximately 30 min after implant, the device automatically checks for AV conduction and switches to AAI mode if appropriate.
Updated MVP algorithm
To answer, some limitations of the first version, the MVP algorithm has been updated in the most recent platforms.
Switch to DDD in case of long PR intervals
The presence of a very long PR interval can be accompanied by a more or less prominent symptomatology. In the first version of the MVP algorithm, the device did not switch in case of long PR intervals. At the request of some physicians faced with patients remaining symptomatic in the setting of long PR on exertion, the algorithm was modified accordingly.
The device monitors the PR (AS-VS) and AR interval (AP-VS). When the average AV interval exceeds a programmable fixed AV limit, the device switches to DDD.
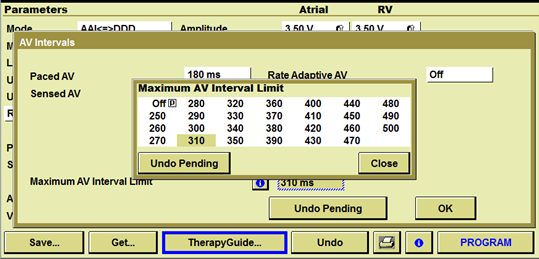
The AV interval limit is programmable. If the patient’s average AV interval exceeds this AV interval limit, the device switches to DDD mode.
In this patient, the AV limit has been programmed at a value of 300 ms: the device switches to DDD when the average AV interval exceeds 300 ms.
The first atrioventricular conduction verification occurs 1 minute after switching to the DDD mode; during this verification, if the PR or AR interval remains prolonged and greater than the programmed value, the device continues in DDD mode; the interval between each conduction control is then doubled (2, 4, 8… minutes to a maximum of 16 hours).
By default, the long PR function of the MVP algorithm is programmed OFF.
Reduction of the ventricular pause following AV block
In the initial version of the MVP algorithm, the ventricular pause following AV block could potentially generate symptoms and may infrequently lead to pause-dependent ventricular arrhythmia. The most significant change to the updated version is that the device does not wait until the next atrial event to detect loss of AV conduction. If the expected ventricular sensed signal is late, relative to recent AV conducted events, the device will pace the atrium and then pace the ventricle with a short AV delay of 80 ms.
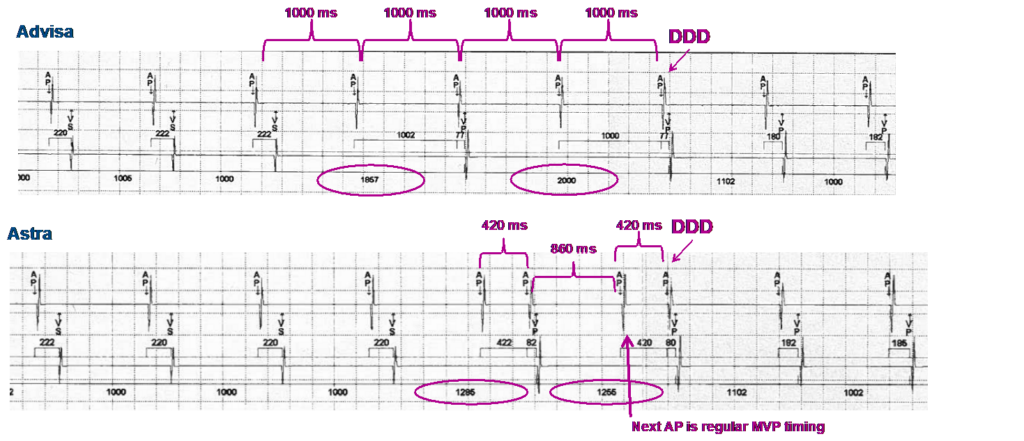
This figure shows the difference in terms of ventricular pause with the 2 versions of the MVP algorithm.
The device analyzes the successive PR intervals (AP-VS or AS-VS); if the atrioventricular conduction is altered (absence of an R wave in a variable window depending on the previous PR intervals), the atrium is paced at least 420 ms, 600 ms at most, after the “blocked” atrial activity (spontaneous or paced). The duration of the AA interval is contingent on the previous measurements of the PR intervals (420 ms if PR < 320 ms). If the PR interval > 320 ms, the AA interval will be longer by 100 ms up to a the limit of 600 ms (for example, if average PR interval is 400 ms, AA interval 500 ms). The timing is the same no matter if the prior AV sequences were AP-VS or AS-VS. Ventricular pacing is subsequently delivered 80 ms after atrial pacing.
The aim of this sequence (atrial pacing prior to ventricular pacing) is to avoid the occurrence of a pause while maintaining atrioventricular synchrony to prevent retrograde conduction and thus reduce the risk of pacemaker-mediated tachycardia. The minimal AA delay of 420 ms also avoids pacing in an atrial vulnerable period and avoids induction of atrial arrhythmias
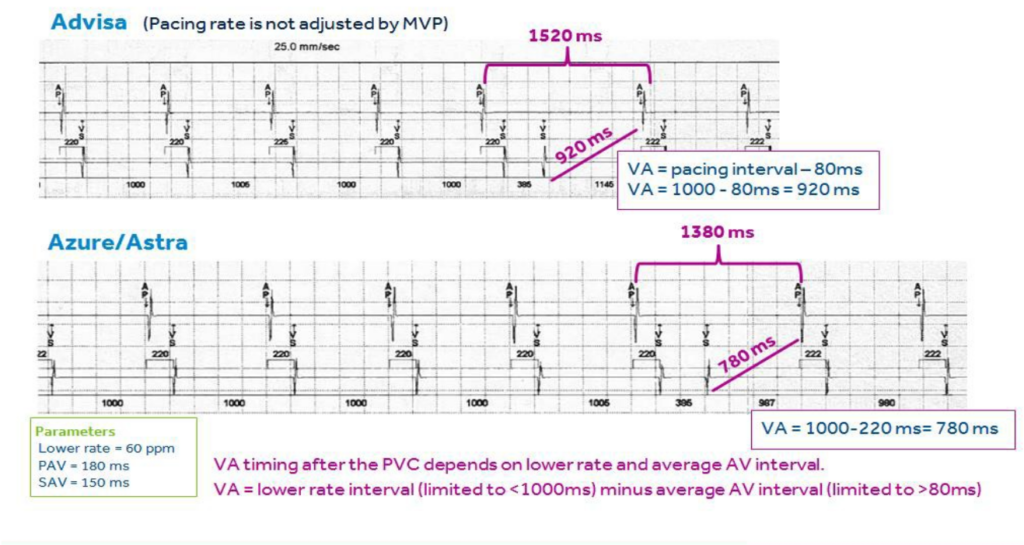
Reduction of the maximal ventricular pause following PVC: VA timing is adjusted (based on previous event timing) to achieve a minimum VV interval of 1000 ms when a PVC occurs. The history of AV intervals is used to determine the VA interval to reduce the pause following PVCs. VA timing is adjusted (based on event timing history) to achieve a shorter pause after ventricular backup paces.
Conduction check: to avoid repetition of conduction check in patients with frequent episodes of AV block. If a successful conduction check occurs, but the device switches back to DDD(R) within 15 seconds, then the conduction check is re-classified as failure and the conduction test interval is not reset to 1 minute, but remains at its current setting.
Delay conduction check at high rates: to avoid the occurrence of blocked P-wave during exercise, if the sensor rate is greater than 90 bpm and the average AR interval is greater than 300 ms, the conduction check is delayed for 1 minute. If the conditions are still met after 1 minute, the conduction check is delayed again for 1 minute.
Crossblanking: the ventricular blanking following atrial pacing has been decreased from 30 ms to 10 ms to reduce the risk of undersensing of a late PVC.
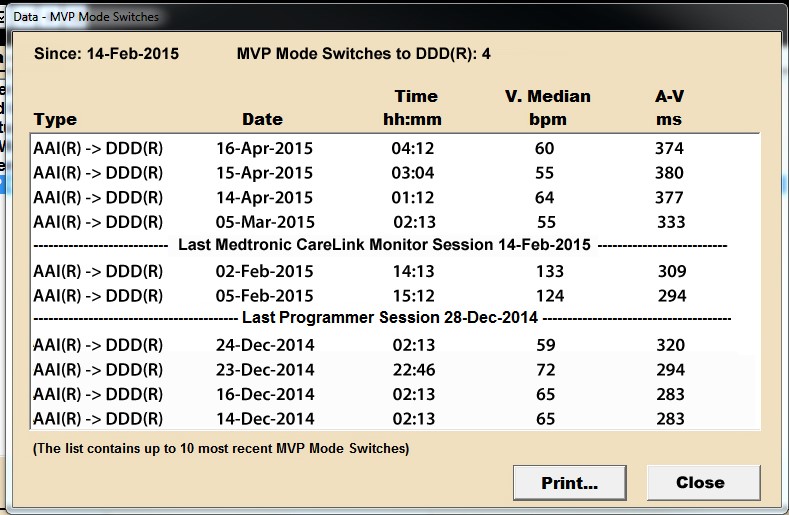
MVP mode switches diagnostic: the diagnostic log was added to understand the nature and frequency of the mode switches. The device maintains the 10 most recent MVP Mode Switches to DDD and a count of MVP Mode Switches since the last session. The most recent MVP Mode Switch Log records the following information when the device, programmed to an MVP pacing mode, switches from AAI to DDD mode:
- Type of mode switch
- Date and time when the mode switch occurred
- Median ventricular rate at the time of the mode switch
- AV interval at the time of the mode switch