Medtronic Discrimination
Specificities
When programming an ICD, particular attention should be paid to the risk of inappropriate therapies. Modern ICD offer several advanced criteria, which, alone or combined, can discriminate VT from SVT. The “heart rate” criterion cannot be used safely alone, as its specificity for the diagnosis of ventricular tachyarrhythmias is only 60%, while its sensitivity can be easily increased to 100%. Moreover, the lower the programmed VT zone, the lower its specificity. Without other discrimination criteria, the therapy will be delivered irrespective of the origin of the tachycardia. The VF zone is typically reserved for very high rate and left without other intervening criteria, which are used only in the VT zone for patients susceptible of developing very rapid ventricular rates during SVT. These criteria should be deactivated in patients with fixed complete AV block.
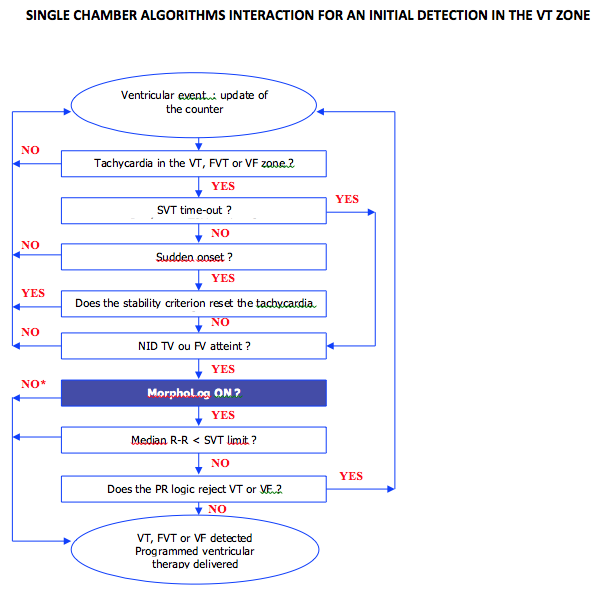
Discrimination in a single-chamber ICD
The discriminating criteria offered by single chamber ICD include sudden onset, stability of the tachycardia cycle length and morphology of the ventricular EGM.
The « sudden onset » criterion withholds therapies for tachycardia of gradual onset, and is typically used to prevent inappropriate therapies for sinus tachycardia. The « stability » criterion limits the delivery of therapy for irregular tachyarrhythmias in the VT zone and is often used to prevent inappropriate therapy for atrial fibrillation with a rapid ventricular rate, which is usually irregular, whereas it is usually regular during VT. “Morphology” is a matching criterion that compares the EGM during tachycardia with that previously recorded during intrinsic rhythm. It is based on the principle that the ventricular EGM should be identical during a rapidly conducted SVT and during sinus rhythm. It compares dynamically ventricular EGM recorded during all episodes of tachycardia in the VT zone with a template previously recorded. If both EGM are classified as similar, the arrhythmia is diagnosed as “supraventricular”.
Onset
Operating details: comparison of an average of the 4 most recent with the average of the 4 previous intervals. As long as the onset is classified as gradual, detection is postponed and the event is marked as VS.
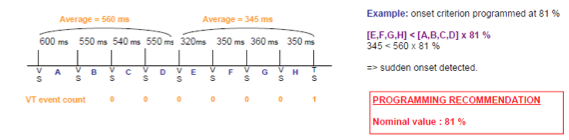
Onset monitor: the device performs all the calculations associated with “onset” though does not delay the detection.
Note: the onset criterion applies to VT and FVT via VT during the initial detection only, and not in redetection.
At onset in the VT zone, the device measures each interval. If the onset is detected as gradual, a) the intervals are classified as VS, b) a “gradual onset” notation appears, and c) the detection is withheld.
Stability
Operating details: stability intervenes when the VT event count reaches 3; an interval is classified as unstable if its length varies from the 3 previous intervals by a difference greater than the programmed stability interval. If the device detects an unstable interval, SVT is detected and the VT event counter is reset to 0.
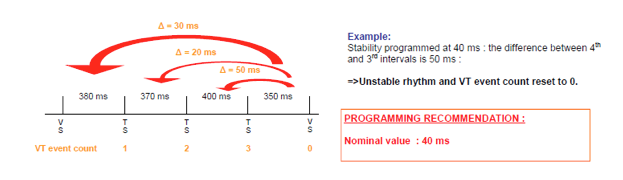
Note : The stability criterion applies to VT and FVT via VT during initial detection and redetection.
When the VT event counter reaches 3, the stability criterion is fulfilled.
If the event is classified unstable, a) it is marked as a normal sensed event (VS), b) the VT event counter is reset to 0 and starts ‘Re-Counting’, and c) a “Stability” notation appears.
Wavelet
Operating details: compares the 8 QRS preceding the detection of a tachycardia with a stored template (reference morphology). If ≥6 of the last 8 QRS do not match the stored template, VT is detected; if ≥3 of the last 8 QRS match the stored template, the VT event counter is reset to 0 and therapy is withheld.
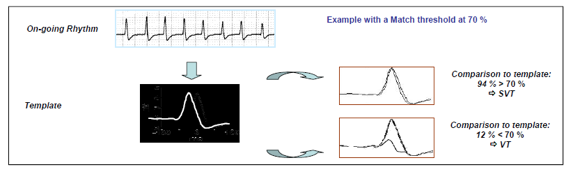
Programmable settings : On, Off, Monitor
Match threshold : 40, 43, …, 70, …, 97%
Auto sampling : On (sampling every 17 min), Off
Wavelet rules
-
Template sampling and conditions
The template can be sampled automatically:
Sampling of 6 normal sinus rhythm complexes and creation of a template based on their average. The automatic template is validated by a comparison of the 6 waveforms among each other (at least 4 out of 6 must match)
Template confirmation: one waveform is sampled every 10 s and compared to the stored template over 700 s. If ≥70 out of 100 waveforms match the template, it is confirmed.
Regular verification of the template quality: samples a waveform every 17 min (~1000 s) and compares to the stored template.
- Wavelet sampling trigger
Wavelet starts to sample if:
The VT event count = 2
The VF event count = 3
Wavelet begins its comparison with the stored template 2 events later.
-
Wavelet interruption
Episode detection: ≥6 of the last 8 waveforms do not match to the stored template
High rate time out
Episode end: rate >VT interval
Wavelet applies only when the median V-V interval is ≥SVT limit.
Wavelet uses EGM 2: HVA to HVB (Can to RV coil) source. If the printed peak-to-peak amplitude of the R wave is <3 mV, a different EGM 2 source must be chosen. If the base-to-peak amplitude is >6 mV, consider increasing the EGM 2 range.
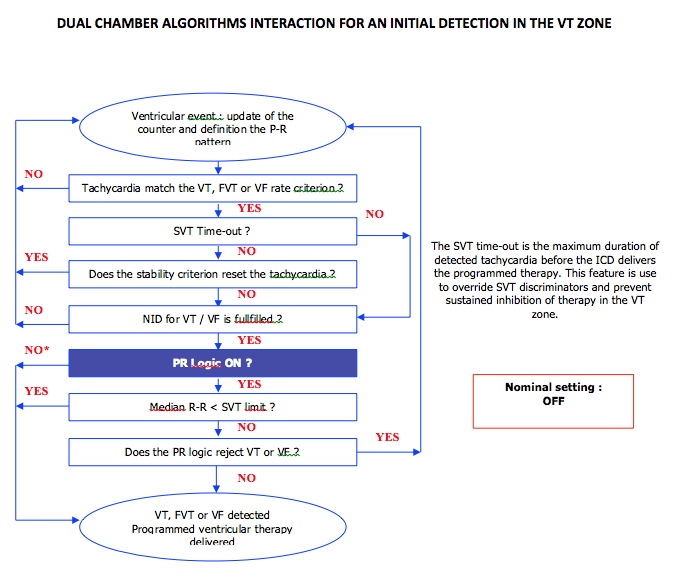
Discrimination in a dual- triple-chamber ICD
Operating details: permanent and simultaneous scrutiny of 6 criteria. When the number of intervals (NID) to detect VT or VF is reached, the following diagnostic rules are applied.
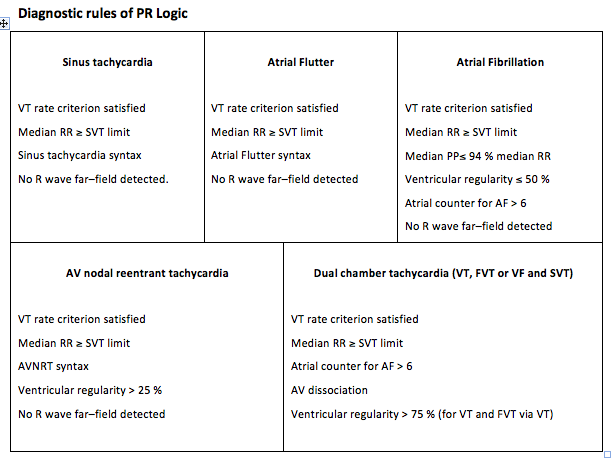
PR Logic operates only on initial detection and not on redetection;
PR Logic operates only for rates below the programmed SVT limit.
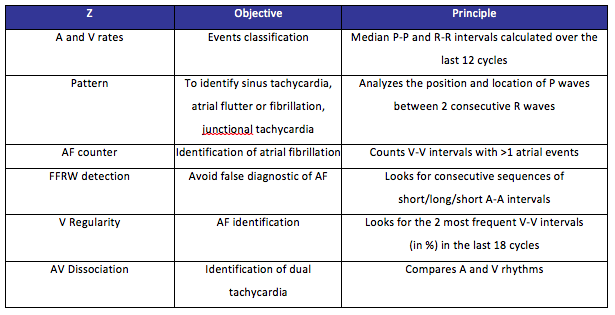
Pattern
Analyzes beat-to-beat in real time
Looks for the position and sequence of P waves among 3 consecutives R waves
Assigns a code to each observed sequence
Compares the codes with 19 different pre-stored patterns to identify a potential SVT
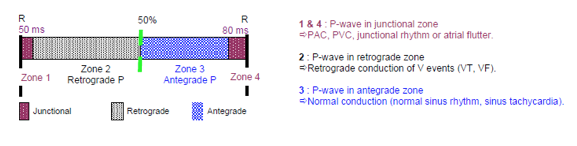
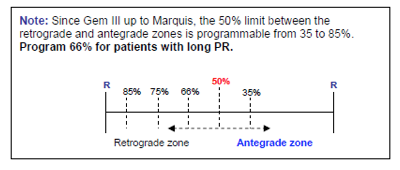
AF detection
Goal: identify atrial fibrillation or dual-tachycardia
Algorithm:
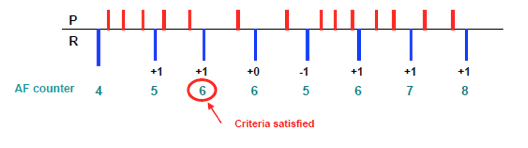
≥2 atrial signals within 1 RR interval => Counter +1
No atrial signal within 1 RR interval => Counter –1
1 atrial signal within 1 RR interval => Counter –1 if RR stable => Counter +0 if RR unstable
The AF criterion is initially satisfied when the AF counter is ≥6. If the AF criterion is satisfied the therapy is not delivered as long as the counter remains ≥5. The AF counter is limited to a maximal value of 10.
The AF evidence counter analysis determines that an atrial tachyarrhythmia is present if the counter reaches a predefined threshold. Satisfied first at 6, remains satisfied at ≥5, max 10, min 0.
Far-field R wave detection
Operating details: PR Logic identifies a far-field R wave (FFRW) if it simultaneously detects: Successive sequences of “short-long” AA intervals with ≥30 ms differences
A <60 ms AV OR <160 ms VA interval
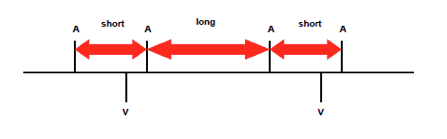
In order to recognize a rhythm as ST with FFRW, it has to be present:
In 10 of the last 12 intervals in Gem DR devices
Starting with Gem III DR and later models, it was decreased to 4 of the last 12 intervals
AV dissociation
Operating details: AV-dissociation is confirmed if 1 of the following is present in ≥4 of the last 8 V-V intervals:
No atrium
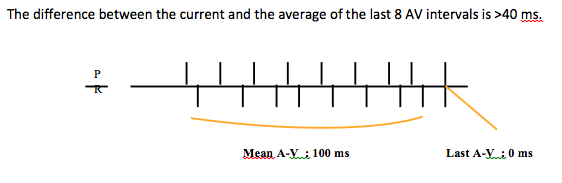
Ventricular regularity
Purpose: identification of atrial fibrillation.
Conducted AF => Irregular ventricular rhythm
Ventricular Tachycardia => Regular rhythm
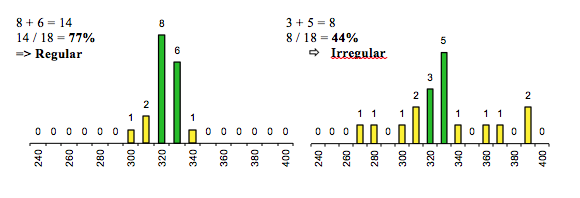
Operating details: calculates the proportion of the 2 most common intervals within the last 18 V-V intervals.
Regularity >75% = regular rhythm
Regularity ≤50% = irregular rhythm
Note: only intervals ≥240 ms in duration are used in this analysis.
Discrimination Smart-shock
Smart-Shock was implemented in the latest generation devices and includes the algorithms T-wave discrimination, RV lead noise discrimination, LIA combined PR Logic + wavelet and discrimination +.
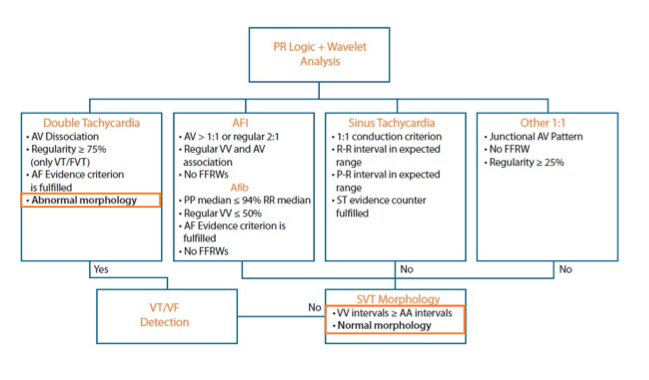
Combined PR Logic + Wavelet
Purpose: combines morphology and A-V pattern recognition to better discriminate all SVT in dual and triple chambers devices.
Confirmation +
This algorithm:
Confirms the heart rhythm is still fast immediately after the delivery of ATP or before a first shock.
Diverts a non-committed therapy before completion of the capacitor charge if the tachycardia ends spontaneously only for the fisrt shock.